Hair Loss: Practical Causes, Treatments, and What Actually Works
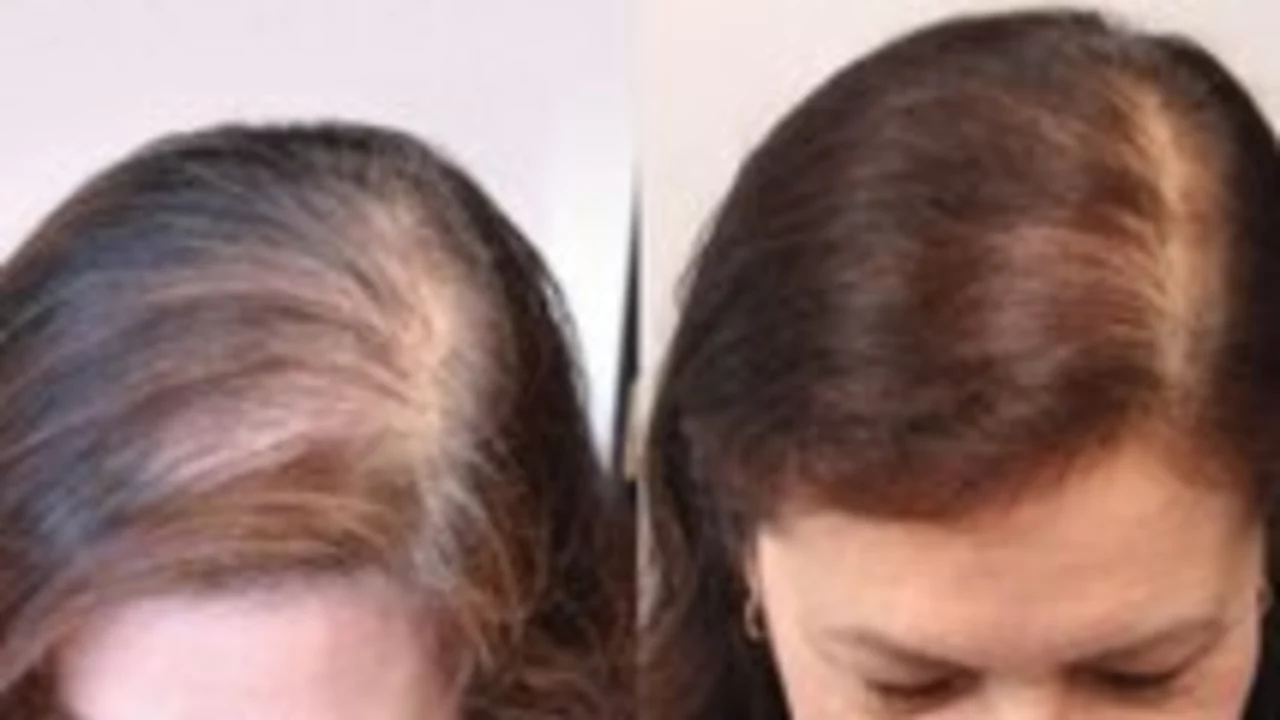
Want to stop losing hair or at least slow it down? You're not alone—about half of people experience noticeable hair loss by middle age. This guide gives clear, usable steps you can try today, and tells you when to see a doctor.
What causes hair loss?
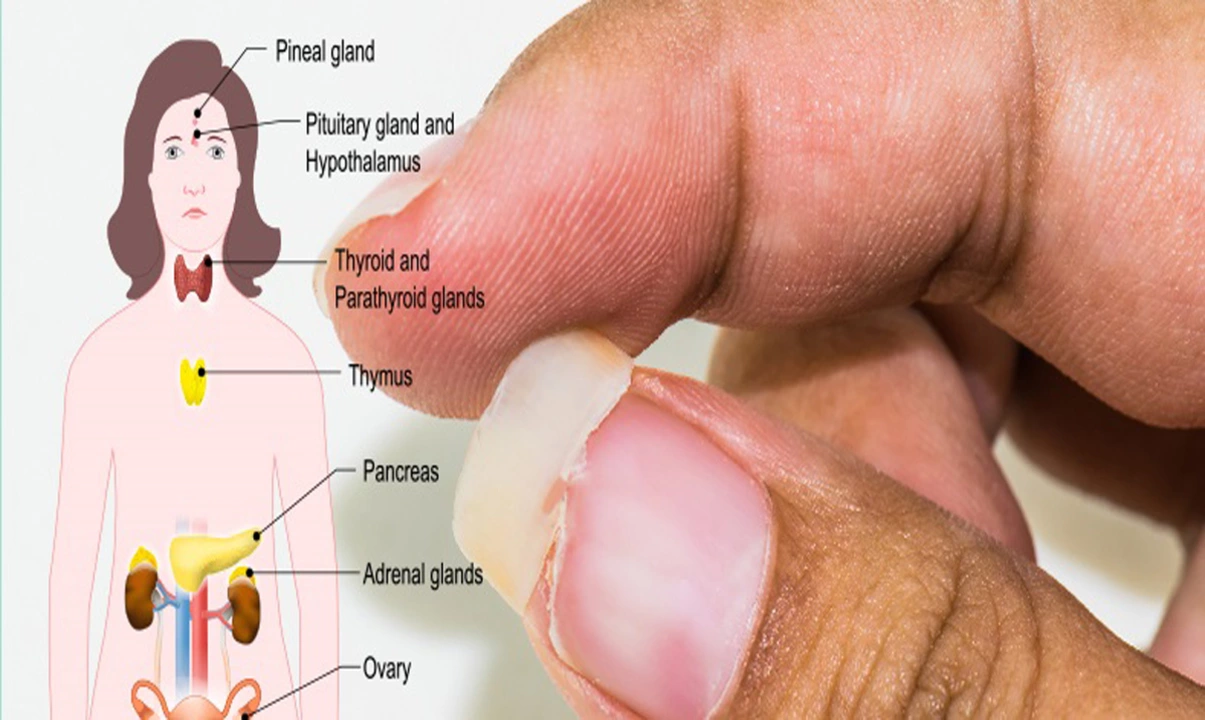
The most common cause is genetics: androgenetic alopecia affects men and women and follows family patterns. Hormones matter too—thyroid problems, pregnancy, and menopause can trigger shedding. Certain medicines—like some blood pressure drugs, antidepressants, and chemotherapy—can cause hair loss. Stress and sudden weight loss can lead to telogen effluvium, a temporary, heavy shed that often recovers in months. Poor nutrition, especially low iron, vitamin D, or protein, also weakens hair.
Treatment options that work
Topical minoxidil is a first-line, over-the-counter option for many types of hair loss. Applied daily, it can slow shedding and stimulate regrowth in some people after a few months. For men with male-pattern baldness, oral finasteride can be effective but has possible sexual side effects—talk to a doctor first. Low-level laser devices and platelet-rich plasma (PRP) injections show promise for some patients, though results vary and costs can be high. Hair transplant surgery moves follicles from dense areas to thin spots and gives permanent, natural-looking results if done well.
Small lifestyle fixes help a lot. Use a gentle shampoo, avoid tight hairstyles that pull on roots, and limit hot tools. Eat a balanced diet with enough protein, iron, and vitamin D; consider a basic multivitamin if your diet is poor. If you suspect a medication is the cause, don't stop it abruptly—discuss alternatives with your prescriber. Stress management—sleep, short walks, and breathing exercises—can cut down on shedding from telogen effluvium.
When should you see a professional? If hair loss is sudden, patchy, or follows a rash or pain on the scalp, book a doctor visit. Also see a dermatologist if you're losing hair fast, if family treatments fail after 6 months, or if you notice other symptoms like weight change or fatigue that might point to thyroid or autoimmune issues. A dermatologist can offer tests—blood work, scalp biopsy, or trichoscopy—to find the exact cause.
Real expectations matter. Most treatments need months to show benefit and may only stop further loss rather than fully restore hair. Combining approaches—topical therapy, improving nutrition, and treating underlying conditions—often gives the best outcomes. If you want to hide thinning while waiting for results, styling tricks, thicker shampoos, or a skilled barber can make a big difference fast.
Ready to act? Start with a basic check: review your meds, get blood tests for iron and thyroid, and try a gentle routine plus minoxidil if appropriate. Keep notes and photos so you can track progress. If you need help choosing next steps, a dermatologist can map out a plan tailored to your situation.
Small changes now can protect future hair—start simple, track results, and ask a pro if you're worried. Quick action often brings better outcomes. Act today now.