When your stomach suddenly locks up in intense pain, lasting for hours, and no amount of antacids or walking it off helps - it might not be indigestion. It could be gallstones. For millions of people, this isn’t a rare condition. In fact, about 1 in 10 adults in the U.S. and Europe has them. But here’s the twist: 80% of those people never even know it. The problem starts when the stones move - and that’s when things get serious.
What Happens When a Gallstone Gets Stuck?
Gallstones form when bile in your gallbladder hardens into pebble-like deposits. Most are made of cholesterol (80% in Western countries), while others are made of bilirubin, a waste product from broken-down red blood cells. They sit quietly until something triggers them - usually a fatty meal. That’s when the gallbladder contracts to push bile into the small intestine. If a stone blocks the cystic duct, bile backs up. The gallbladder swells. And that’s when you feel it: a deep, steady ache under your right ribs or in the middle of your belly.
This pain - called biliary colic is the episodic pain caused by temporary blockage of the cystic duct by a gallstone - doesn’t come and go like cramps. It hits hard, peaks within an hour, and lasts 1 to 5 hours. You can’t relieve it by passing gas, vomiting, or changing positions. And unlike heartburn or gas, it doesn’t respond to over-the-counter meds. That’s a red flag.
Here’s what most people don’t realize: if you’ve had one episode of biliary colic, you’re almost guaranteed to have more. The American Academy of Family Physicians found that over 90% of people have another attack within 10 years. Two-thirds get hit again within just two years. That’s not bad luck - it’s the nature of the disease. The stone doesn’t disappear. It just waits.
When It Gets Worse: Cholecystitis and Beyond
If the blockage lasts more than a few hours, the gallbladder gets inflamed. That’s acute cholecystitis inflammation of the gallbladder due to prolonged obstruction by a gallstone. This isn’t just pain anymore. You’ll likely have a fever, nausea, vomiting, and tenderness so severe you can’t even breathe deeply. The skin around your right side might turn yellow - a sign the stone has moved into the common bile duct and is blocking bile flow. That’s called choledocholithiasis the presence of gallstones in the common bile duct. It can lead to jaundice, infection, or even pancreatitis if the stone blocks the pancreatic duct.
And here’s the scary part: without treatment, 20-30% of people with symptomatic gallstones end up in the emergency room within five years. That’s not a small risk. That’s a ticking clock. The NHS reports that emergency gallbladder surgery is far more dangerous than planned surgery. Conversion from laparoscopic to open surgery jumps from 5% to 25% when inflammation is severe. Recovery takes weeks instead of days. The risk of infection, bleeding, and bile leaks skyrockets.
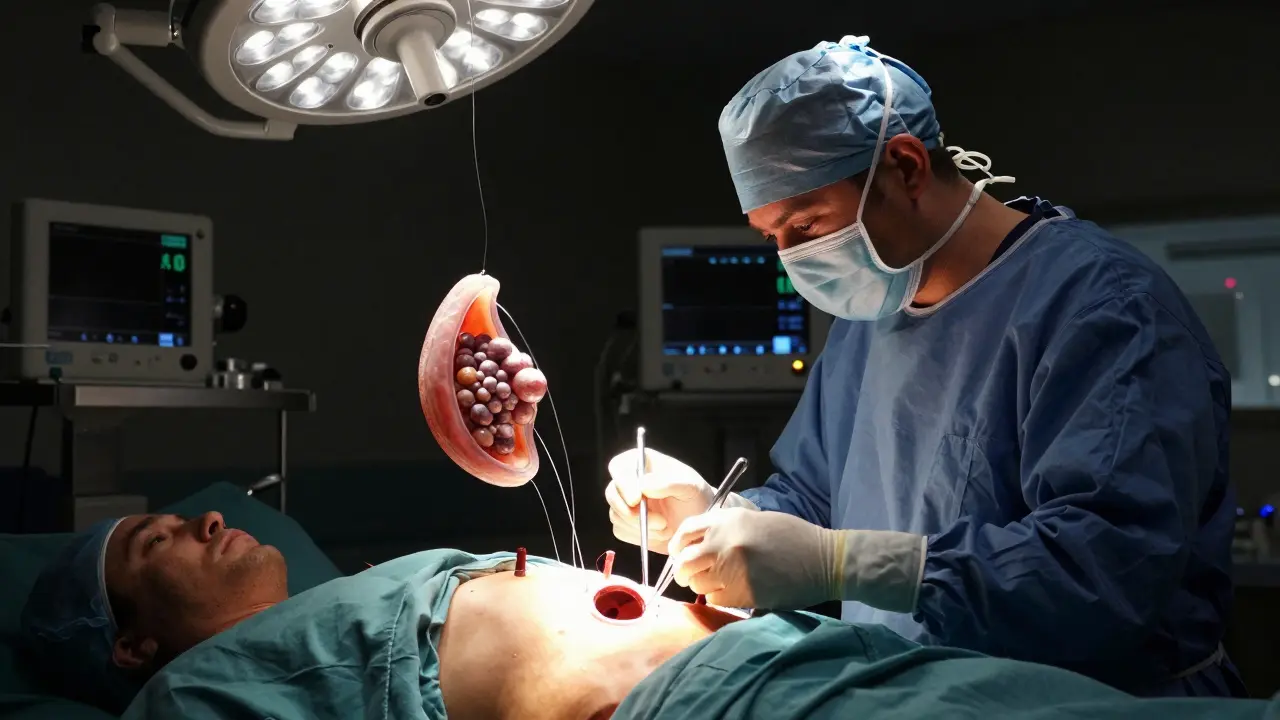
The Gold Standard: Laparoscopic Cholecystectomy
So what’s the fix? For most people, it’s surgery. Not always. But if you’ve had symptoms, the odds are stacked against waiting. The laparoscopic cholecystectomy a minimally invasive surgical procedure to remove the gallbladder using small incisions and a camera is the go-to. It’s done in 90% of cases in the U.S. today. Four tiny cuts. A camera. A few tools. The gallbladder is pulled out like a deflated balloon. Most people go home the same day or the next.
Compare that to open surgery - a big cut under the ribs. Recovery? Four to six weeks. Hospital stay? Nearly five days. Pain? Much worse. That’s why open surgery is now rare - only used when there’s severe scarring, infection, or anatomy too messed up for the laparoscopic approach.
Here’s what patients say. A Healthline survey of over 1,200 people found 78% chose surgery after just three episodes of pain. The biggest reason? Emergency visits. “I thought it was just bad indigestion,” said one 42-year-old woman. “I ended up in the ER with a fever and couldn’t move. I didn’t want to go through that again.”
And the results? Most people feel better within days. A Cleveland Clinic case study followed a woman who had 17 attacks over 18 months. After surgery, her pain vanished in 10 days. She was back to running by week two. On Reddit, 82% of people who had laparoscopic surgery said their quality of life improved dramatically. The only common side effect? Diarrhea - about 1 in 8 people. It usually clears up in a few months as the body adjusts to bile flowing directly into the intestine.
What About Non-Surgical Options?
You’ve probably heard about pills that dissolve gallstones. Or shock waves that break them up. They sound great. But here’s the truth: they’re not the answer for most people.
Ursodeoxycholic acid a bile acid medication used to dissolve small cholesterol gallstones works - but only on tiny, pure cholesterol stones. Success rate? 30-50%. And it takes 6 to 24 months. Even then, half the people get stones back within five years. It’s not a cure. It’s a delay.
Shock-wave lithotripsy? It used to be popular. A machine zaps the stone until it breaks into tiny pieces. Then you take pills to dissolve the fragments. Sounds cool. But it’s messy. Stones often reform. The procedure is expensive. And it’s rarely done anymore. Harvard Health called it “largely outdated” in 2022.
There’s also a new trick: endoscopic ultrasound-guided drainage. The FDA approved it in 2023. It’s for people too sick for surgery - like those with heart failure, advanced cancer, or severe lung disease. A tiny tube is inserted through the skin into the gallbladder to drain it. It’s not permanent. But it buys time. For most people? Surgery is still faster, safer, and more reliable.
Who Should Skip Surgery?
Not everyone needs it. If you’ve never had symptoms, you don’t need surgery. Period. No exceptions.
But what about older adults? That’s where it gets tricky. A 2023 study in the Annals of Surgery found that for patients over 75 with three or more chronic conditions - diabetes, heart disease, kidney problems - the 30-day death risk after surgery jumps from 0.1% to 2.8%. That’s 28 times higher. So for someone frail, with multiple health issues, doctors might say: “Let’s manage the pain. Don’t risk the cut.”
But here’s the catch: even in older people, if they’re otherwise healthy, surgery still has a 95% satisfaction rate. The problem isn’t age. It’s frailty. That’s why experts now use tools to measure “biological age,” not calendar age. Are you strong? Active? Eating well? Then surgery is still the best option - even at 80.

What to Expect Before and After Surgery
Pre-op: You’ll get an ultrasound or CT scan. Blood tests. Maybe an MRI to check if stones are in the bile duct. If you’re overweight, your surgeon might ask you to lose 5-10% of your weight. Why? Less fat around the liver makes surgery easier and safer. If you have diabetes, they’ll get your blood sugar under control. It’s not about being “perfect.” It’s about reducing risk.
On the day: You’ll fast for 8 hours. You’ll get anesthesia. The surgery takes 45 to 60 minutes. Most people wake up with mild shoulder pain (from the gas used to inflate the belly during surgery). It fades in a day.
After: You’ll walk within 4 hours. Drink water within 6 hours. Go home in 24 hours. You’ll feel tired for a few days. No heavy lifting for 2 weeks. Most people are back to work in 7 days. And yes - you can eat normally. Your body adapts. No special diet needed. Just avoid greasy food for the first week while your system recalibrates.
Why So Many People Delay - And Why That’s Dangerous
One of the biggest problems? Misdiagnosis. A Healthline survey found 41% of patients saw three or more doctors before getting the right answer. Gallstones mimic heartburn, gas, even a heart attack. ER doctors miss it. Primary care docs shrug it off. People go home with antacids. And the stone keeps moving.
And then there’s the pain management gap. 29% of patients said they were given inadequate pain relief during attacks. That’s unacceptable. NSAIDs like ketorolac work just as well as opioids - with fewer side effects. But many hospitals still default to narcotics. That’s outdated.
The bottom line: if you’ve had biliary colic, don’t wait. Don’t hope it goes away. It won’t. And each episode increases your chance of emergency surgery - which is riskier, more expensive, and harder on your body. The NHS says untreated gallstones lead to hospitalization in 20-30% of cases within five years. That’s not a gamble. That’s a guarantee.
The future? Surgeons are refining techniques. Single-incision laparoscopic surgery is growing - but it’s riskier. Enhanced recovery protocols are cutting hospital stays by 30%. And research continues into better ways to predict who’s at risk. But for now? The answer hasn’t changed: if you have symptoms, remove the gallbladder. It’s not just about pain. It’s about preventing the next crisis.
Can gallstones go away on their own?
No. Gallstones don’t dissolve or disappear without treatment. If they’re not causing symptoms, they may stay harmless. But once they start causing pain - like biliary colic - they will keep causing problems. The stone doesn’t vanish. It just waits for the next trigger.
Is gallbladder surgery risky?
For healthy people, laparoscopic cholecystectomy is one of the safest major surgeries. Complication rates are below 2% in experienced hands. The biggest risks come when surgery is delayed - leading to emergency procedures. In those cases, complications like infection, bile leaks, or needing open surgery rise sharply.
Do I need to change my diet after gallbladder removal?
You don’t need a special diet long-term. For the first week, avoid very fatty or fried foods - your body is adjusting to bile flowing directly into the intestine. Most people return to their normal diet within a month. Some may have looser stools for a few months, but that usually improves on its own.
What are the alternatives to surgery?
Medications like ursodeoxycholic acid can dissolve small cholesterol stones, but only in about half of cases - and it takes over a year. Stones return in half of those patients within five years. Shock wave therapy and drainage tubes exist, but they’re temporary fixes. Surgery remains the only permanent solution for symptomatic gallstones.
Why do women get gallstones more often than men?
Estrogen increases cholesterol in bile and slows gallbladder emptying. That’s why women - especially those who’ve been pregnant, use birth control, or take hormone therapy - are 2 to 3 times more likely to develop gallstones. Genetics, obesity, and rapid weight loss also play roles.
How do I know if I need surgery?
If you’ve had one episode of biliary colic - especially if it was severe, lasted more than a few hours, or required ER care - surgery is strongly recommended. Waiting increases your risk of complications like cholecystitis or pancreatitis. Talk to a surgeon. Don’t wait for the next attack.






Comments(8)